Immunizations remain one of the most effective and cost-efficient public health interventions available. Recognized by the U.S. Public Health Service as one of the Ten Great Public Health Achievements of the 20th Century, vaccines have played a critical role in reducing—and in some cases eliminating—life-threatening diseases. As vaccine recommendations evolve, staying informed is essential to protecting both individual and community health.
Vaccines protect not only those who receive them, but also strengthen community-wide immunity, particularly for infants, older adults, and individuals with compromised immune systems. High vaccination rates reduce the spread of preventable diseases and help avoid outbreaks that can strain healthcare systems and disproportionately impact vulnerable populations.
Understanding Vaccine Recommendations

Prior to 2026, children were recommended to receive a series of routine immunizations that protected against serious illnesses such as measles, polio, whooping cough, hepatitis B, and pneumonia. This schedule commonly referred to as 4:3:1:3:3:1:4, included:
- 4 doses of DTaP (diphtheria, tetanus, pertussis)
- 3 doses of polio
- 1 dose of MMR (measles, mumps, rubella)
- 3 doses of Hib
- 3 doses of hepatitis B
- 1 dose of varicella
- 4 doses of pneumococcal vaccine
These recommendations were grounded in decades of research and continuous safety monitoring that ensured vaccines were both safe and effective during early childhood.

Recent Changes and What They Mean for Families
Public health experts note that some changes aim to align U.S. recommendations with international vaccination standards. In response, the American Academy of Pediatrics (AAP) raised concerns about the changes departed from long-standing, evidence-based standards that were informed by a limited review of international practices and emphasized the importance of rigorous scientific review to ensure clear and consistent recommendations for families and healthcare providers.
For parents and caregivers, these updates may raise questions. Open communication and evidence-based information are essential to informed decision-making.

Beyond the Numbers: A Community Responsibility

Vaccine recommendation changes affect health equity. Vaccines not on the recommended schedule lack insurance coverage, creating financial barriers for families. These gaps disproportionately affect low-income households and communities with limited access to preventive care, highlighting the need for equitable, evidence-based immunization policies.
While immunization data helps guide public health policy, behind every statistic is a child, a family, and a community. Vaccination is not only a personal health decision—it is a shared responsibility that helps protect the most vulnerable, including infants, seniors, and those with weakened immune systems, by reducing the spread of preventable illness throughout our communities.
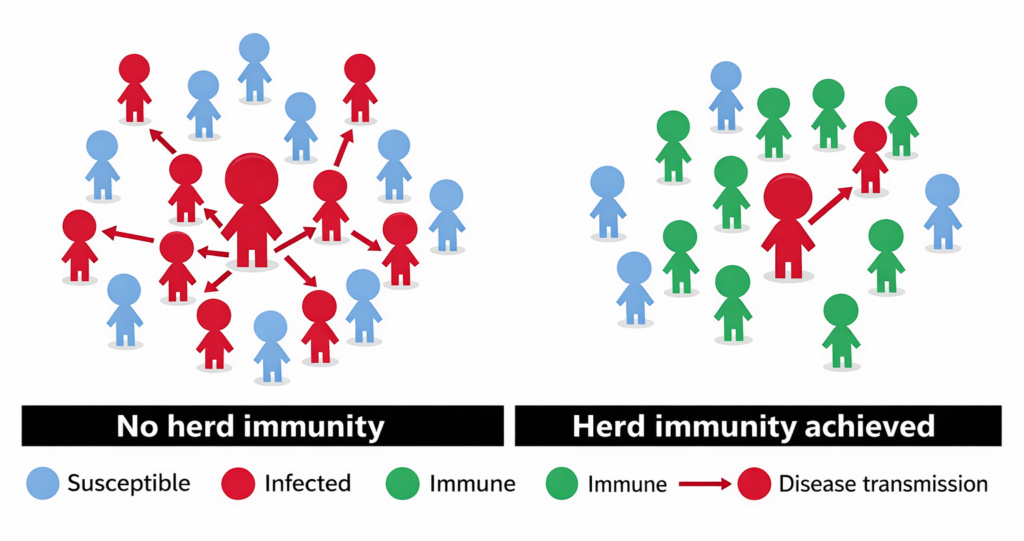
Vaccinating children and adults protects more than just the individual—it safeguards the entire community, especially those most vulnerable. High vaccination coverage slows or stops the spread of contagious diseases, prevents outbreaks, and reduces severe illness, hospitalization, and death. It shields infants, people with weakened immune systems, the elderly, and others who cannot be fully vaccinated, creating a protective “community immunity.” Maintaining widespread vaccination also keeps diseases from returning and protects future generations. Every vaccinated person plays a role in strengthening the community’s immunity and protecting those at higher risk.